Feedback on Snake Bite: A Small Puncture Can Create a Large Problem
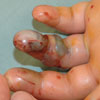
I enjoyed the case involving an 8-year-old boy whose hand was bitten by a copperhead snake1 but would point out the following inaccuracies.
The authors erroneously state that CroFab (the antivenin used to treat the patient) is "obtained by fractionating blood from healthy horses immunized with the venom of 4 different species of poisonous snakes." Horse serum was used in the older antivenin formulations and it was unfractionated. CroFab is based on fractionated ovine serum, thus decreasing the possibility for anaphylaxis or other allergic reaction.
Regarding the ambiguous statement, "It [CroFab] is only indicated for the treatment of envenomation caused by bites of the crotalids (pit vipers) that are specified." CroFab does not have antibody specifically against copperhead venom; it is made of antibodies to 3 types of rattlesnake and 1 type of water moccasin. It should have good effect—at the very least—against North American crota-lid venoms.
The authors note that "venomous snakes have a distinctly triangular head with elliptical pupils and pits as well as nostrils." This morphology is only true of pit vipers, however. The statement holds mostly true for North America and South America, where most of the poisonous snakes are pit vipers. The exception is the coral snake, which evolves neurotoxic venom. It has a rounded head and is better typified by its red, yellow, and black banding pattern. Coral snakes are usually found in the southern United States and throughout South America. It is important to differentiate this snake from others because envenomation, though rare, requires very specific antivenin. The bite from even a juvenile coral snake is more than adequate to kill a full-grown man.
This case bears an important message. For those of us who grew up around copperheads, the accepted wisdom has been that the venom is quite weak and that injury and death are rare. In fact, the consequences of a copperhead bite depend on the site of the bite. Bites to the feet and hands require close observation and quick intervention if worrisome signs develop.
——Michael Wittkamp MD
Department of Pediatrics
Chinle Comprehensive Health Care Facility
Indian Health Service
Chinle, Ariz
The authors have contributed an interesting case of snake venom poisoning. I would point out, however, that some of their statements perpetuate several incorrect, long-repeated recommendations about venomous snake bites.
The authors write that pit viper toxin is hemotoxic and that it consists of proteins and peptides (among other constituents). Pit viper venom is a more accurate term; however, venoms contain numerous components, including toxins of several classes. Also, the term "hemotoxic" is far too general because most crotaline viperids (the pit vipers are a subfamily [crotaline] of the viper family [Viperidae]) secrete venoms that contain vasculotoxins (ie, proteolytic rhexic hemorrhage), indirect hemolysins (phospholipases A), thrombin homologues, platelet inhibitors, and bradykinin-potentiating peptides. Almost all of these toxins are polypeptides, which (by definition) are proteins.
Of more concern is the often repeated attempt to classify a given venom as "hemotoxic" or "neurotoxic" This is incorrect and clinically misleading because there are many additional venom components with varying pharmacological activities. Some crotaline venoms also contain Mojave toxin or related isotoxins. These are potent presynaptic neurotoxins. Envenomation inflicted by a rattlesnake with Mojave toxin in its venom may manifest itself with minimal local effects, progressive paresis, and cardiorespiratory collapse.1 Some North American crotaline venoms also contain myotoxins and thus may also produce rhabdomyolysis.2 The authors' discussion would have been better served if their comments were restricted to a review on copperhead envenoming.
The authors mention the use of a suction device "if available" within 30 minutes of a bite. Such devices are highly controversial3; thus, their use can only be justified when an envenoming occurs in a remote location and an exceptionally delayed intervention or evacuation is anticipated. Use of pressure/immobilization could be considered for envenomings inflicted by neurotoxic populations of the Mojave rattlesnake and possibly those by coral snakes. However, this technique—used primarily in Australia—has an unproven role in crotaline envenomings and may be harmful because of the exacerbation of local effects of hemorrhagic/cytotoxic crotaline venoms.4
The authors list several morphological characteristics of "venomous snakes," including head and pupillary shape and the presence of a rattle. Many small harmless nocturnal snakes have elliptical pupils and some harmless water snakes have large heads that might appear triangular to the uninitiated. Many rattlesnakes lose their rattle segments and, less commonly, their entire rattle. Cottonmouths do not have a rattle, and although almost never involved in snake bites, there is a rattle-less rattlesnake (the Catalina island rattlesnake, Crotalus catalinensis).
The key message is any loose guidelines for distinguishing venomous snakes from nonvenomous ones are likely to be incorrect, confusing, and potentially dangerous. If the snake is killed, it should be brought with the patient for identification by a qualified person. As there is a significant danger of being bitten, however, the capture by an unqualified person of a specimen involved in an envenoming cannot be endorsed.
——Scott A. Weinstein, PhD, MD
Bayside, NY
We thank Drs Wittkamp and Weinstein for these clarifications. We gathered general information on snake bites from the references cited in our article and from information obtained from our Children's Hospital poison center, the toxicology department, and the CroFab package insert. Our article was not meant to be an in-depth study of North American snake bites. The brief case study focused on a brave and resilient 8-year-old boy who received timely and excellent treatment from EMS, MedFlight, emergency department staff, hand surgeons, and wonderful nurses. Because of the correct diagnosis and timely treatment, not only was this patient's finger saved, but he has regained the full function of his finger.
——Pamela Horn
CRNP Program Coordinator for Orthopedics Clinical Services Care
Coordination Children's Hospital
Columbus, Ohio
1. Horn P, Popp JE, Dimitris KD, Ruth B. Snake bite: a small puncture can create a large problem. Consultant For Pediatricians. 2007;6:297-302.
2. Norris R. Venom poisoning by North American reptiles. In: Campbell JA, Lamar WW, eds. The Venomous Reptiles of the Western Hemisphere. Vol 2. Ithaca, NY: Cornell University Press; 2004:683-708.
3. Carroll RR, Hall EL, Kitchens CS. Canebrake rattlesnake envenomation. Ann Emerg Med. 1997;30:45-48.
4. Bush SP, Hegewald KG, Green SM, et al. Effects of a negative pressure venom extraction device (Extractor) on local tissue injury after artificial rattlesnake envenomation in a porcine model. Wilderness Environ Med. 2000;11:180-188.
5. Sutherland SK, Coulter AR, Harris RD. Rationalisation of first-aid measures for elapid snakebite. Lancet. 1979;1:183-185.


