Painful Oral Lesions: What to Look For, How to Treat, Part 1
Author:
Jeffrey A. Burgess, DDS, MSD
Seattle
Citation:
Burgess JA. Painful oral lesions: what to look for, how to treat, part 1. Consultant. 2006;46(13):1497-1504.
ABSTRACT: Risk factors for oral cancer include tobacco use and alcohol intake (especially in conjunction with tobacco use). Many benign conditions may be confused with squamous cell carcinoma, the most common type of intraoral neoplasm. Any red and/or white lesion that has surface corrugation, stippling, or induration is considered dysplastic or neoplastic until proved otherwise. Even without these clinical signs, white plaques of any size that persist for several months may represent dysplasia. These lesions should be assessed by biopsy. Risk factors for lichen planus include stress, exposure to certain foods and medications, and systemic illness. Erosive lichen planus may cause significant pain and oral dysfunction.
KEYWORDS: benign neoplasms, intraoral lesions, squamous cell carcinoma, lichen planus
Malignant oral lesions—particularly in their early stages—can resemble benign conditions. In this 2-part series, I will offer practical advice on how to identify symptomatic lesions. Here I focus on oral cancer and lichen planus. In a future article, I will discuss viral infections, candidiasis, benign mucous membrane pemphigoid, and erythema multiforme.
ORAL CANCER
Oral squamous cell carcinoma accounts for about 3% of all cancers in the United States. Risk increases with age, although recent years have seen a trend toward increasing prevalence in younger men. Oral squamous cell carcinoma affects more men than women, and risk varies according to country and race. In the United States, the incidence is about 12.3% in blacks, 10% in whites, 5.7% in Hispanics, and 6% in Asians. Mortality is about 4.8% in blacks, 2.5% in whites, 2.3% in Asians, and 1.3% in Hispanics.1 The overall 5-year survival rate is about 50%. This relatively low rate is largely attributable to delayed diagnosis of an initially innocuous-appearing, asymptomatic lesion in a location difficult for the patient and clinician to observe readily.1
_________________________________________________________________________________________________________________________________________
Related Content
White Oral Lesions: How to Distinguish the Benign From the Deadly
A Mouthful of Oral Lesions
_________________________________________________________________________________________________________________________________________
Risk factors for oral malignancy. These include heavy cigarette smoking and the use of smokeless tobacco; alcohol intake (especially when coupled with tobacco use); low serum levels of β-carotene; radiation therapy; iron deficiency; infection with oncogenic viruses, including human papillomavirus (HPV) and herpes simplex virus (HSV); immunosuppression; and the activity of proto-oncogenes, tumor suppressor genes, and gatekeeper molecules in association with alcohol and tobacco use.2 The mechanisms and interactions involved in malignant transformation are complex, but the result of the combination of environmental factors and genetics is defective carcinogen metabolism and cellular DNA repair capabilities, which lead to tumor growth.
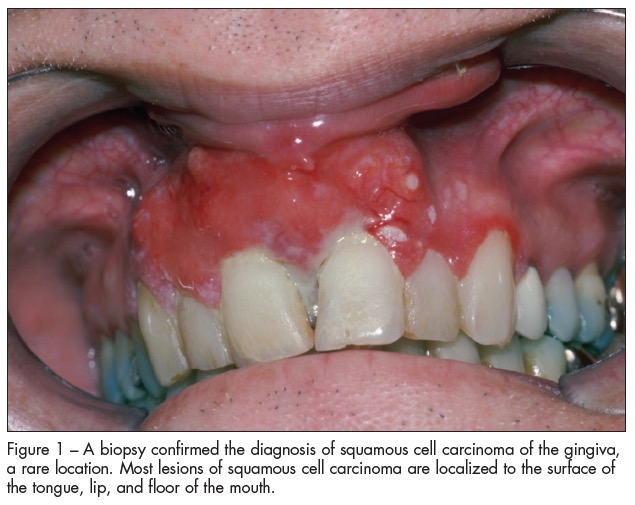
Clinical features. The most common type of intraoral neoplasm is squamous cell carcinoma; others include oral adenocarcinoma, Kaposi sarcoma, and melanoma. The last 3 conditions do not generally involve pain. About 85% of oral carcinomas arise on the lips, tongue, oropharynx, and floor of the mouth. Rarely, squamous cell carcinoma may present on the soft palate and attached gingival tissue (Figure 1). Pain is not often the presenting feature, although patients may complain of an "irritation" or "sore." Initial signs include a change in color of the normally pink epithelium to red (erythroplakia or erythroplasia), red/white (patchy erythema), or white (leukoplakia) (Figure 2); ulceration and/or erosion; a change in surface texture (eg, stippling or corrugation); and, in advanced cases, induration of the peripheral area of the lesion, failure to heal, and neck lymphadenopathy.3

Any red and/or white lesion that presents with surface corrugation, stippling, or induration is considered dysplastic or neoplastic until proved otherwise. White plaque of any size that persists for several months may be dysplastic even if it does not display these clinical characteristics. It should be assessed by biopsy because of the risk of malignant transformation. Past or current snuff or tobacco use may predispose a user to epithelial neoplastic transformation.
Although oral squamous cell carcinoma typically presents as a single lesion, a number of reports suggest that persons with this disease are at increased risk for future oral malignancy.4,5 In one study, 19% of patients with oral cancer observed at 1 year were found to have new primary cancers.6 Thus, continued thorough assessment of the mouth is warranted in patients in whom the initial presentation of squamous cell carcinoma is a solitary lesion.
Tongue malignancy typically involves the anterior two thirds of the lateral and ventral surfaces. Small lesions may be aggressive and quickly invade the musculature. Consequently, nodal metastases may occur early in the course of the disease.7 The importance of early detection cannot be overemphasized, given that mortality is highly correlated with metastasis. About 60% to 70% of cancer deaths related to tongue malignancy follow recurrence of tongue lesions. Only 15% of deaths are the result of distant metastases, and 20% to 40% are related to second primary cancers.8,9
Tumors that arise on the floor of the mouth may spread to adjacent tongue and gingival tissue. Lesions in this area are aggressive, and examination may reveal submandibular and cervical nodal involvement. If these nodes are fixed to the mandible, suspect periosteal involvement, possible bone invasion, and advanced disease. Advanced squamous cell carcinoma that involves the gingiva may also cause teeth to loosen as a result of bone destruction.
Five-year survival for patients with squamous cell carcinoma depends on the site of the malignancy and the length of time the lesion has been present. If a lesion remains localized and does not invade the basement membrane, survival increases dramatically. Significant morbidity is associated with attempts to prolong survival. For tongue lesions, survival is dramatically increased if there is no nodal involvement at presentation.10
NEXT: Differential Diagnosis of Oral Cancer
Differential diagnosis. Benign conditions that may resemble squamous cell carcinoma include benign hyperkeratosis, lichen planus, lichenoid drug reaction, Behçet disease, major aphthae, erythematous candidiasis, areata migrans (geographic tongue), papilloma, verruca vulgaris, and chemical or medicinal burns. Snuff keratosis, a premalignant condition, presents as a generalized whitening coupled with surface corrugation (Figure 3). A high transformation rate has been demonstrated in these lesions.

Diagnostic procedures. In addition to history, clinical presentation, and tissue biopsy, a number of procedures may be useful in assessing for oral cancer. Toluidine blue dye in a 1% aqueous solution applied over a small area with a cotton swab or a larger area via rinse is a simple tool used to assess excessive mitotic activity or mucopolysaccharide production, findings that suggest squamous cell carcinoma.11
Another potentially useful procedure--exfoliative cytology--involves removal of cells with a cytology brush. This painless procedure is reported to have high sensitivity and specificity.12 The technique is particularly useful in patients who require repeated procedures in multiple sites.13 Incisional biopsy remains the gold standard for evaluation of potential malignancy.
Prevention and treatment. Several recent developments may affect future intervention strategies for squamous cell carcinoma. In the early 1980s, HPV was linked to anogenital squamous cancer; this led to research on the potential effect of HPVs on squamous cell carcinoma. Accumulating evidence points to a link between HPV-16 and squamous cell carcinoma of the head and neck; the strongest evidence is for a link between the virus and carcinoma of the tonsil.14 Although the specific mechanisms involved in HPV-induced carcinoma have not been fully elucidated, evidence suggests that a vaccine might prevent tonsillar cancer.15,16 In May 2006 the FDA advisory committee recommended the use of a vaccine found to be effective against HPV subtypes 16, 18, 6, and 11. HPV-16 has been the most common isolate in oral dysplasia and carcinoma.17 Further research will determine whether this vaccine might prevent intraoral squamous cell carcinoma.
CO2 laser surgery is a potentially useful approach for generalized surface hyperplasia with multiple areas of dysplasia when excisional biopsy is not appropriate. A caveat is that tissue is destroyed and not collected for evaluation. In one 4-year study, 76% of patients who underwent this surgery for oral cancer prevention remained disease-free.18
NEXT: Lichen Planus
LICHEN PLANUS
This condition is one of the most common disorders of the oral mucosa, but it is frequently misdiagnosed largely because it has 6 subtypes and a variety of presentations. The incidence of this benign disorder is less than 1%. The prevalence increases with age, and women are affected slightly more often than men. Lichen planus may also involve the glabrous skin, hair, and nails.19-21 It rarely affects children.22
Clinical features. The variants of oral lichen planus are categorized according to morphology. The most common type, reticular lichen planus (Figure 4), presents as a slightly rough, whitened, elevated surface plaque; as a lace-like pattern (Wickham striae); or as asymptomatic papules or plaques.Single or multiple lesions may involve the lip, attached gingiva, or unattached mucosa of the cheek, tongue, soft or hard palate, or floor of the mouth.

Erosive or ulcerative lichen planus (Figure 5) can manifest as an isolated lesion or affect a considerable area with significant pain and oral dysfunction. In both reticular and erosive/ulcerative lichen planus, intraoral lesions may occur with or without generalized cutaneous involvement.23,24 For some patients the condition is quite dynamic, with episodic remission and recrudescence or with a change from reticular to erosive presentation. In about 0.4% to 3% of cases, lichen planus converts to squamous cell carcinoma.25

Risk factors. These include stress, exposure to certain foods (eg, cinnamic acid and aldehyde in chewing gum); dental amalgam (typically from older fillings or fillings adjacent to gold crowns);and systemic illness (such as graft versus host disease and liver disease). A lichenoid drug reaction may be provoked by medications, including NSAIDs, angiotensin-converting enzyme inhibitors, thiazide diuretics, β-blockers, phenothiazines, tetracyclines, and carbamazepine. Others have been implicated.26 A relationship between lichen planus and hepatitis C has been suggested.27 Interestingly, this appears more common in the Mediterranean countries and in Japan, which suggests immunogenetic or geographic factors.28,29
Diagnosis and follow-up. The erosive and ulcerative variants of lichen planus are the most likely to undergo malignant transformation. Hence, patients with this clinical presentation require annual assessments and periodic biopsy.Tissue sampling through biopsy also helps differentiate lichen planus from a number of other disorders that have a similar clinical presentation. These include chronic ulcerative stomatitis; pemphigus; benign mucous membrane pemphigoid (BMMP) (cicatricial pemphigoid); dermatitis herpetiformis; systemic lupus erythematosus; allergic reactions; and chronic responses to infection, such as atrophic candidiasis. Although standard hematoxylin and eosin processing of a tissue sample may suffice to rule out a neoplasm, differentiation of lichen planus from other immunologic conditions, such as BMMP and pemphigus, may require direct immunofluorescent analysis.
Treatment. Empirical treatments of lichen planus include antimicrobials (eg, antibiotics, antifungals, antimalarials, and antivirals); immunomodulators (eg, topical and systemic corticosteroids); cytotoxic agents; hormones; immunostimulants (eg, levamisole); immunosuppressants (eg, cyclosporine); retinoids such as etretinate and isotretinoin; surgery (eg, cryotherapy, laser surgery, conventional surgery); and UV radiation (eg, psoralen-UV-A). Medications have been used topically or delivered systemically or by injection, depending on the extent of disease and type of drug being administered. Treatment decisions are a function of the extent and duration of the condition, confounding secondary abnormality (such as infection), the presence of dysplasia, the patient's history, and cost.
Reticular lichen planus does not require treatment unless there are cosmetic concerns (eg, lip involvement). Mild cases of erosive or ulcerative lichen planus can be managed with topical corticosteroids (fluocinonide gel or ointment 0.05%, clobetasol propionate gel or ointment 0.05%) or an elixir of 0.5 mg/5 mL dexamethasone. Oral candidiasis may be controlled by coadministration of an antifungal agent. In severe cases, a methylprednisolone dose pack or higher dose prednisone regimen with rapid taper can be used, followed by continuation of topical corticosteroid therapy. Azathioprine, 50 to 100 mg/d, is an effective long-term treatment for refractory erosive lichen planus.
Dr Burgess was clinical assistant professor at the University of Washington Dental School in Seattle and a consultant/attending physician at the University of Washington Medical Center Pain Center for more than 15 years. He is currently in private practice. In a previous article (CONSULTANT, January 2006, page 25), Dr Burgess reviewed nondental conditions that cause orofacial pain, such as temporal arteritis, trigeminal neuralgia, burning mouth syndrome, postherpetic neuralgia, and salivary gland pathology.
NEXT: References

REFERENCES:
- Silverman S, Eversole R. Oral premalignancies and squamous cell carcinoma. In: Silverman S, Eversole R, Truelove E, eds. Essentials of Oral Medicine. London: BC Decker Inc; 2002.
- Batsakis J, ed. Tumors of the Head and Neck, Clinical and Pathological Considerations. 2nd ed. Baltimore: Williams and Wilkins; 198
- Silverman S Jr, ed. Oral Cancer. Atlanta: American Cancer Society; 1981.
- Sciubba JJ. Oral cancer: the importance of early diagnosis and treatment. Am J Clin Dermatol. 2001;2:239-251.
- Tabor MP, Brakenhoff RH, Ruijter-Schippers HJ, et al. Multiple head and neck tumors frequently originate from a single preneoplastic lesion. Am J Pathol. 2002;161:1051-1060.
- Silverman S, Griffith M. Smoking characteristics of patients with oral carcinoma and the risk for second primary oral carcinoma. J Am Dent Assoc. 1972;85:637-640.
- Spiro RH. Squamous cancer of the tongue. Cancer. 1985;35:252-256.
- Vermund H, Brennhovd I, Kaalhus O, Poppe E. Incidence and control of occult neck node metastases from squamous cell carcinoma of the anterior two thirds of the tongue. Int J Radiat Oncol Biol Phys. 1984;10:2025-2036.
- Wallner PE, Hanks GE, Kramer S, McLean CJ. Patterns of care study: analysis of outcome survey data—anterior two thirds of tongue and floor of mouth. Am J Clin Oncol. 1986;9:50-57.
- Zwetyenga N, Majoufre-Lefebvre C, Siberchicot F, et al. Squamous cell carcinoma of the tongue: treatment results and prognosis. Rev Stomatol Chir Maxillofac. 2003;104:10-17.
- Zhang L, Williams M, Poh CF, et al. Toluidine blue staining identifies high-risk primary oral premalignant lesions with poor outcome. Cancer Res. 2005;65:8017-8021.
- Pektas ZO, Keskin A, Gunhan O, Karslioglu Y. Evaluation of nuclear morphometry and DNA ploidy status for detection of malignant and premalignant oral lesions: quantitative cytologic assessment and review of methods for cytomorphometric measurements. J Oral Maxillofac Surg. 2006;64:628-635.
- Maraki D, Becker J, Boecking A. Cytologic and DNA-cytometric very early diagnosis of oral cancer. J Oral Pathol Med. 2004;33:398-404.
- Hobbs CG, Sterne JA, Bailey M, et al. Human papillomavirus and head and neck cancer: a systematic review and meta-analysis. Clin Otolaryngol. 2006;31:259-266.
- Billish J. HPV vaccine MedImmune/GlaxoSmithKline. Curr Opin Investig Drugs. 2003;4:210-213.
- Connett H. HPV vaccine moves into late stage trials. Nature Medicine. 2001;7:388.
- Watts SL, Brewer EE, Fry TL. Human papillomavirus DNA types in squamous cell carcinomas of the head and neck. Oral Surg Oral Med Oral Pathol. 1991;71:701-707.
- Thomson PJ, Wylie J. Interventional laser surgery: an effective surgical and diagnostic tool in oral precancer management. Int J Oral Maxillofac Surg. 2002;31:145-153.
- DiFede O, Belfiore P, Cabibi D, et al. Unexpectedly high frequency of genital involvement in women with clinical and histological features of oral lichen planus. Acta Derm Venereol. 2006;86:428-433.
- Bouquot JE, Gorlin RJ. Leukoplakia, lichen planus, and other keratoses in 23,616 white Americans over the age of 35 years. Oral Surg Oral Med Oral Pathol. 1986;61:373-381.
- Boyd AS, Neldner KH. Continuing medical education: lichen planus. J Am Acad Dermatol. 1991;25:593-619.
- Milligan A, Graham-Brown R. Lichen planus in children—review of six cases. Clin Experimental Dermatol. 1990;15:340-342.
- Bhattacharya M, Kaur I, Kumar B. Lichen planus: a clinical and epidemiological study. J Dermatol. 2000;27:576-582.
- Schwartz MP, Sigurdsson V, Vreuls W, et al. Two siblings with lichen planus and squamous cell carcinoma of the esophagus. Eur J Gastroenterol Hepatol. 2006;18:1111-1115.
- Scully C, Beyli M, Ferreiro MC, et al. Update on oral lichen planus: etiopathogenesis and management. Crit Rev Oral Biol Med. 1998;9:86-112.
- McCartan B, McCreary C. Oral lichenoid drug eruptions. Oral Dis. 1997;3:58-63.
- Sanchez-Perez J, Castro M, Buezo G, et al. Lichen planus and hepatitis C virus: prevalence and clinical presentation of patients with lichen planus and hepatitis C virus infection. Brit J Dermatol. 1996;134:715-719.
- Carrozzo M, Brancatello F, Dametto E, et al. Hepatitis C virus-associated oral lichen planus: is the geographical heterogeneity related to HLA-DR6? J Oral Pathol Med. 2005;34:204-208.
- Lodi G, Biuliani M, Majorana A, et al. Lichen planus and hepatitis C virus: a multicentre study of patients with oral lesions and a systematic review. Br J Dermatol. 2004;151:1172-1181.
EVIDENCE-BASED MEDICINE:
• Eisen D. the clinical features, malignant potential, and systemic associations of oral lichen planus: a study of 723 patients. J Am Acad Dermatol. 2002;46:207-214.
• Ingafou M, Leao JC, Porter SR, Scully C. Oral lichen planus: a retrospective study of 690 British patients. Oral Dis. 2006;12:463-468.
• Sciubba JJ. Oral cancer: the importance of early diagnosis and treatment. Am J Clin Dermatol. 2001;2:239-251.
FOR MORE INFORMATION:
• www.oralcancerfoundation.org
• www.cancer.gov/cancertopics/wyntk/oral
• www.aafp.org/afp/20000601/3319.html
• www.aocd.org/skin/dermatologic_diseases/lichen_planus.html
Therapeutic Agents in This Article
Acyclovir (Zovirax)
Azathioprine (Imuran)
Carbamazepine (Tegretol)
Clobetasol (Temovate, Cormax, Embeline E)
Clotrimazole (Cruex, Lotrimin, Desenex)
Dapsone
Dexamethasone (Aeroseb-Dex, Decaspray, Decadron)
Etretinate (Tegison)
Fluconazole (Diflucan)
Fluocinonide (Fluonex, Lidex)
Isotretinoin (Accutane)
Ketoconazole (Nizoral)
Levamisole (Ergamisol)
Methylprednisolone (Medrol)
Nystatin (Mycostatin, Nilstat, Nystex)
Prednisone (Deltasone, Orasone, Panasol-S)
Tetracycline (Sumycin)


